EU/EEA falls short on TB detection as one in five cases go unnoticed
Ahead of World Tuberculosis Day new report shows that Europe needs to do more to reach 2030 targets
A new joint surveillance report from the European Centre for Disease Prevention and Control (ECDC) and the World Health Organization’s (WHO) Europe Office highlights persistent gaps in tuberculosis (TB) detection and care across the Europe Region, which comprises 53 countries.
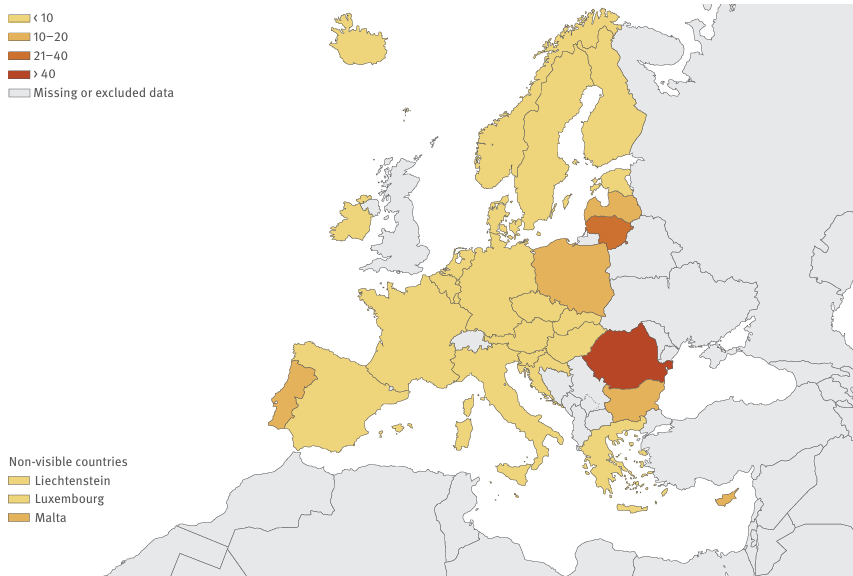
The situation in the 30 EU/EEA countries is better than the wider region, though Romania stands out for particularly elevated levels of the disease. Despite progress over the past decade, the report shows that one in five TB cases in EU/EEA countries still go undiagnosed or unreported, undermining efforts to eliminate the disease.
In 2024, 38,249 TB cases were reported across the EU/EEA, but detection gaps and weak follow-up systems remain major challenges. Notably, 22% of patients who begin treatment are not evaluated after one year, raising concerns about treatment success and ongoing transmission. These gaps are especially worrying for vulnerable groups, including children and people in prison.
“During the past decade, the EU and EEA countries have seen the number of TB cases decrease by 33% and the number of deaths by 17%,” said ECDC Director Dr. Pamela Rendi-Wagner. “To achieve the 2030 targets, continued efforts and collaboration are needed in early detection and sustained follow-up.”
Drug-resistant TB adds further urgency. While 3.5% of TB cases in the EU/EEA are multidrug-resistant, treatment success for these cases is only 56%. Poor outcomes allow resistant strains to persist and spread, making the disease harder and more costly to treat.
WHO Regional Director Dr. Hans Henri P. Kluge stressed the consequences of missed diagnoses: “One in five people with TB in the European Region are still being missed by health services. That is not only a failure in detection, it is a missed chance to treat earlier, prevent suffering and stop further transmission.”
The report calls for intensified early detection, wider use of rapid diagnostics, and stronger patient follow-up. Without these improvements, EU/EEA countries risk falling short of their 2030 TB elimination targets, leaving thousands of preventable infections and deaths each year.
A disease of the past?
Tuberculosis may be less visible in Europe than it once was, but it remains a serious public health threat. Speaking on ECDC’s podcast for World Tuberculosis Day 2026, ECDC TB expert Senia Rosales-Klintz stressed that the disease is far from a relic of the past.
“Tuberculosis still exists in Europe, and that’s something that is important to remember,” she said. Each year, around 40,000 people in Europe are diagnosed. While that is low compared with the global burden, Rosales-Klintz warned that “there is still plenty to do,” especially because TB disproportionately affects people already facing difficult social conditions, living in crowded accommodation or prisons.
She described TB as a disease that can remain hidden in the body for years. “It looks a bit like a hide-and-seek type of game between our immune system and the bacteria”. In some cases, the immune system contains the infection without fully clearing it, allowing the bacteria to lie dormant and re-emerge later, particularly in older people or those with weakened immunity.
Treatment is one of the biggest challenges. Unlike a typical bacterial infection treated with one antibiotic for a few days, TB usually requires four to six months of continuous treatment with at least four medicines. “It is really long in comparison to other bacterial diseases,” Rosales-Klintz said. Patients may begin to feel better before the bacteria are fully eliminated, which makes adherence difficult. If treatment stops for too long, the disease can return and may become resistant to drugs.
'People are dying of tuberculosis in Europe in 2026'
That is when the consequences can become severe. Drug-resistant TB may require more medicines, longer treatment, serious monitoring for side effects and, in some cases, even surgery. Rosales-Klintz gave a stark warning: “People are dying of tuberculosis in Europe in 2026.”
Europe also faces a paradox. Because TB is relatively rare, newer medicines may not be readily available in the EU market. “We are sort of victims of our own success,” she said, explaining that Europe is often not an attractive market for manufacturers. As a result, some newer drugs are not registered locally or are harder and more expensive to obtain.
Unless detection improves, treatment is completed, and access to effective medicines is strengthened, tuberculosis will continue to claim lives in Europe and the risks of antimicrobial resistance increase.
